
When Data Isn’t Enough: Listening to Youth Living With HIV
Written by: Damilola Ayowole, Temitope Oluwadare, Soneye Islamiat & Azees Ayotunde | Team Abeokuta, Nigeria
We have spent years working with numbers, prevalence rates, treatment coverage, viral suppression targets. Data shapes how we understand HIV, how we design programs, and how we measure success. Yet, during the designathon that birthed HIV-In-Colors, we confronted a difficult truth: data alone does not tell the full story of adolescents and young people living with HIV.
That realization became both the greatest challenge and the most important lesson of this project.
The challenge: when evidence feels incomplete
As public health physicians, we are trained to trust evidence. Surveys, indicators, and clinical outcomes guide our decisions. But as we began designing HIV-In-Colors, we felt an uncomfortable gap between what the data said and what young people actually lived.
The numbers told us that adolescents were on treatment. They did not tell us how it felt to hide medication from friends, to fear disclosure at school, or to internalize stigma long after a clinic visit ended. The data showed retention rates; it did not show shame, silence, or resilience.
At the designathon, our initial instinct was to “strengthen psychosocial support” in familiar ways, add counseling sessions, integrate screening tools, train providers. These ideas were evidence-based, but they were also top-down. We were designing for young people, not with them.
That was our first major challenge: unlearning professional certainty.
Learning to listen differently
The designathon forced us to slow down and listen, not through questionnaires, but through stories. Conversations with fellow participants, mentors, and youth advocates pushed us to ask a different question: What if young people could show us their experiences instead of explaining them?
That question reshaped the project.
Photovoice emerged not simply as a research method, but as a listening tool we needed to learn. The idea that adolescents could use images to document stigma, hope, isolation, or healing shifted the balance of power. Instead of extracting information, we created space for expression.
This approach challenged us deeply. As researchers, we value structure, defined tools, measurable outcomes, clear endpoints. Photovoice resists rigidity. It is emotional, unpredictable, and deeply personal. It demanded trust: trust in participants, trust in the process, and trust that meaning could emerge without being forced.

The designathon lesson: Youth are not just beneficiaries
One of the most powerful lessons from the designathon was realizing that youth expertise is not symbolic, it is practical. When adolescents and young people living with HIV became central to the design conversation, the intervention evolved in ways we had not anticipated.
Healing circles, for example, were initially framed as group therapy sessions. Youth feedback transformed them into something broader: safe, recurring spaces for shared silence, laughter, anger, and belonging. The emphasis shifted from “intervention delivery” to community formation.
We learned that stigma is not only external. Many young people spoke about stigma they had absorbed into their self-identity. No survey captured that adequately. Their stories did.
Listening also revealed constraints we might otherwise have overlooked, fear of being photographed, concerns about confidentiality, emotional fatigue. These realities shaped our ethical safeguards and implementation strategies far more effectively than any protocol draft.
When impact is not immediately measurable
Another challenge was resisting the urge to define success too narrowly. In public health, we often prioritize quick wins and easily measurable outcomes. But psychosocial healing does not follow linear timelines.
Some lessons from HIV-In-Colors were subtle: a participant speaking for the first time in a group, someone choosing a metaphor instead of words, another deciding not to share an image publicly, and feeling empowered by that choice.
The designathon helped us recognize that process itself can be impact. Creating a safe space is not a precursor to intervention; it is the intervention.
This reframing was uncomfortable. It required us to accept outcomes that are harder to quantify but no less real.
What we will carry forward
Looking back, the most important lesson from HIV-In-Colors is this: programs fail when we confuse participation with inclusion. Inviting youth to attend sessions is not the same as inviting them to shape meaning.
Listening requires surrender of expertise, of timelines, of control. But it also creates interventions that breathe, adapt, and endure.
The designathon strengthened our belief that innovation in HIV care does not always mean new technology or complex systems. Sometimes, it means creating space for young people to be seen, heard, and trusted as narrators of their own lives.
As we move forward with this project and others, we carry a quieter confidence. We still value data deeply, but we now ask different questions of it. We look for the stories it misses and the voices it cannot capture.
Because when it comes to adolescents and young people living with HIV, listening is not optional, it is the work.


 Congratulations to our 2026 Appreciative Inquiry-Based D&I Course cohort for completing our five-week c
Congratulations to our 2026 Appreciative Inquiry-Based D&I Course cohort for completing our five-week c Sonnen Atinge | iCARE Plus
Sonnen Atinge | iCARE Plus Doreen Kemigisha | MU-JHU
Doreen Kemigisha | MU-JHU Aishat Adedoyin Koledowo | S-ITEST
Aishat Adedoyin Koledowo | S-ITEST Yolanda Mayman | ATTUNE
Yolanda Mayman | ATTUNE Agatha Mnyippembe | MWOTAJI
Agatha Mnyippembe | MWOTAJI
 Gift Ndalumbira | RISE
Gift Ndalumbira | RISE




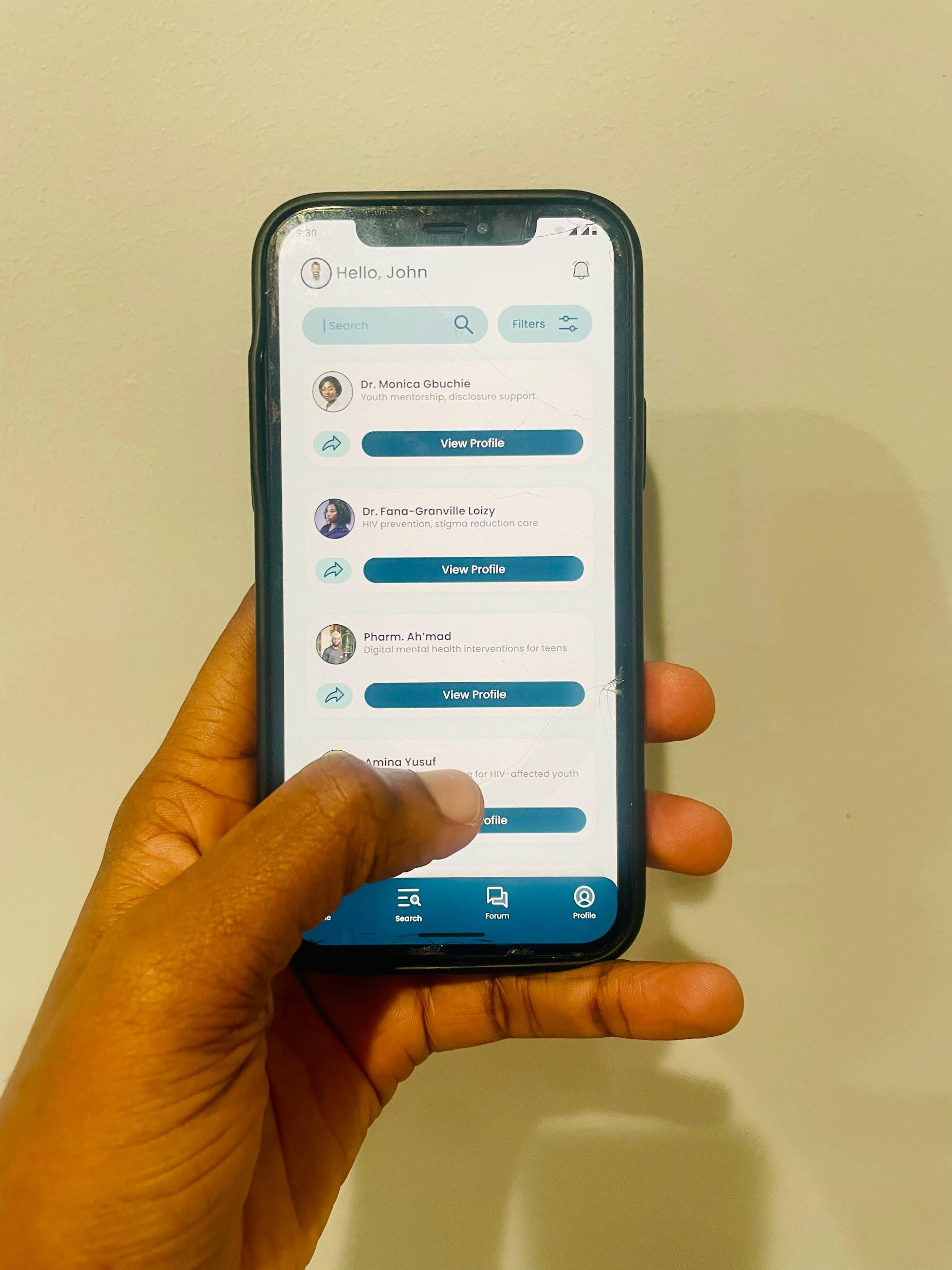



 So far, we have trained peer educators and navigators and carried out a pilot outreach. It hasn’t been entirely smooth—particularly in peri-urban communities. Some challenges we’ve faced include persistent stigma and limited knowledge about HIV testing among youth.
So far, we have trained peer educators and navigators and carried out a pilot outreach. It hasn’t been entirely smooth—particularly in peri-urban communities. Some challenges we’ve faced include persistent stigma and limited knowledge about HIV testing among youth. 